As in so many areas of public health, changes wrought by the COVID-19 pandemic continue to be felt throughout society. And as is often the case, devastation in some areas is balanced by hopeful developments in others.
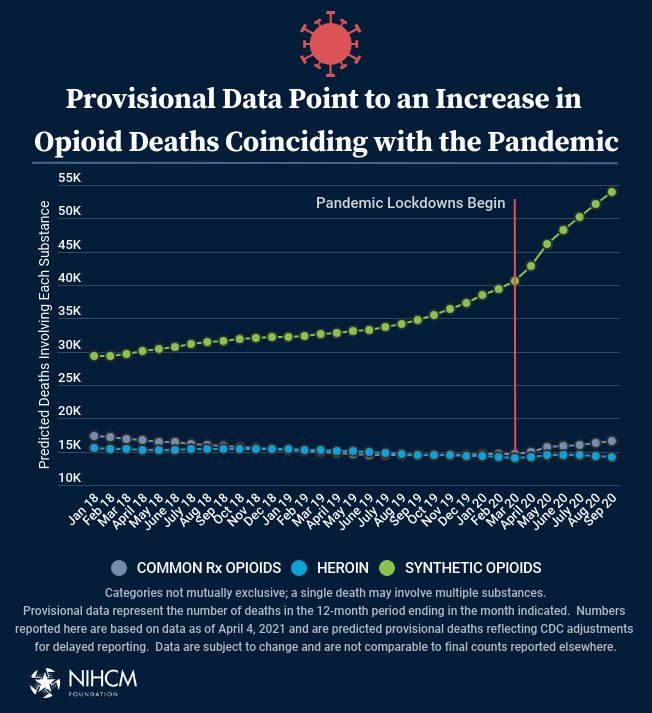
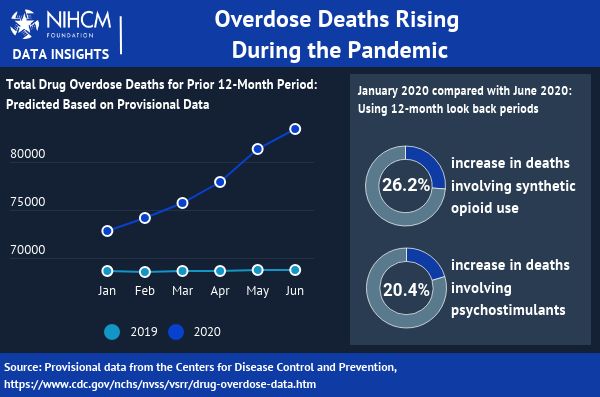
Earlier this month, the Centers for Disease Control and Prevention (CDC) released provisional data from October 2019-September 2020, confirming the fears of many experts that the pandemic has exacerbated the existing drug overdose crisis. Fatal overdoses increased by 29 percent, and those that occurred during the first six months of the pandemic grew at a faster rate than in the six months prior.
Perhaps the most evident and immediate impact of lockdown measures was loss of employment. For many, this created a cascading effect, resulting not just in loss of income, but idle time, loneliness, depression and anxiety, increasing the possibility of using drugs in isolation and the likelihood of a fatal overdose.
Moreover, many drug treatment centers and syringe services programs were forced to temporarily close and/or scale back their hours of operation, greatly impacting the ability of some individuals to maintain their sobriety or practice safer drug use.
Additionally, the worst effects of the crisis have impacted racial/ethnic minorities who were already disproportionately hit hard by COVID-19. In 2019-2020 non-Hispanic Black Americans accounted for the largest increase in opioid-involved deaths by racial/ethnic group, adding to existing evidence that drug overdose mortality was rising fastest among non-Hispanic Blacks prior to the pandemic.
Fortunately, the pandemic has also spurred long-needed changes and innovation in drug treatment, including home delivery of methadone, telehealth outpatient drug treatment groups and telemedicine for buprenorphine treatment. Though racial/ethnic minority disparities persist, these changes have temporarily increased access to treatment for some.
This week, President Biden extended an order to expand buprenorphine prescribing to include certified nurse midwives, anesthetists, and clinical nurse specialists, and to reduce some of the burdensome regulations.
While these are welcome and necessary changes, we have significant work ahead of us to reverse the overdose crisis -- but returning to pre-COVID life is not enough.
In order to effectively address the crisis we need to employ a more robust approach, including a major expansion of medication assisted treatment, particularly to racial and ethnic minorities; expanding evidence-based prevention services, including harm reduction programs; targeted naloxone distribution to individuals at high risk of opioid overdose; and reducing the stigma associated with drug use.
With these and other measures we can counteract the worst of the pandemic with treatment that improves the health and wellbeing of the most vulnerable among us.
Courtney McKnight, DrPH
Clinical Assistant Professor of Epidemiology

Nicolas Geiman
Bachelor of Science Candidate in Global Public Health & Biology